Dr. Nina Kraus on Why Musical Training Helps us Process the World Around Us
https://medium.com/the-kennedy-center/dr-nina-kraus-on-why-musical-training-helps-us-process-the-world-around-us-6962b42cdf44
Sent from Flipboard

(SAN FRANCISCO) — The National Cancer Institute (NCI) of the US National Institutes of Health has designated BrainHQ online brain exercises, made by Posit Science, as a part of its "Research-Tested Intervention Programs" (RTIPs). BrainHQ is now included in the NCI database of evidence-based cancer interventions and program materials for program planners and public health practitioners.
The RTIPs program was set up by NCI to more rapidly move new science into "programs for people." It is a searchable database to help practitioners and program planners find evidence-based interventions that have sufficient relevance to be considered for use in real-world settings.
BrainHQ was selected for inclusion into the RTIPs program because it was tested in research studies, produced positive behavioral and psychosocial findings in cancer survivors, and study results were published in peer-reviewed medical journals. These findings were independently reviewed and scored by NCI and its partners as part of the process by which BrainHQ was included in the RTIPs program.
In selecting BrainHQ for RTIPs, NCI looked at published studies on the use of BrainHQ to address common complaints of cognitive impairment associated with cancer and its treatment. These cognitive impairments are often referred to as "cancer-induced cognitive impairment" or, more colloquially, as "chemobrain." Up to 90 percent of cancer survivors report cognitive issues from cancer or its treatment. There is no widely-accepted treatment for chemobrain.
NCI reviewed an 82-person randomized controlled trial conducted at the University of Indiana, which found that those who used a set of visual processing exercises now found in BrainHQ showed improvements, as compared to the control group, in objective measures of processing speed and verbal memory, as well as on standard measures of perceived cognitive functioning, symptom distress (anxiety, mood, fatigue), and quality of life. NCI also took note of a 242-person pragmatic study led by researchers at the University of Sydney in Australia, which found improvements compared to the control group in self-reported cognitive symptoms, symptom distress, and quality of life.
"We are honored that BrainHQ has been selected by the National Cancer Institute for inclusion in the Research-Tested Intervention Programs," said Dr. Henry Mahncke, CEO of Posit Science. "It is our mission to get scientific breakthroughs like brain-plasticity-based training out of the research lab and into the hands of people it can help. That crucially depends on groups like NCI RTIPs to qualitatively evaluate the level of evidence in new scientific fields, so that program planners and public health practitioners can deliver services that improve people's lives. "
There are now more than 100 peer-reviewed medical and science journal articles on the benefits of Posit Science exercises and assessments, across varied populations. BrainHQ exercises have been shown to improve standard measures of cognition (speed, attention, memory), quality of life (mood, confidence, health-related quality of life) and real-world activities (gait, balance, driving) in healthy adults.
About Posit Science
Posit Science is the leading provider of clinically proven brain fitness training. Its exercises, available online at www.BrainHQ.com, have been shown to significantly improve brain speed, attention, memory and numerous standard measures of quality of life in multiple studies published in more than 60 peer-reviewed articles in leading science and medical journals. Three public television documentaries as well as numerous stories on news programs, in national magazines, and in major newspapers have featured Posit Science's work. The company's science team is led by renowned neuroscientist Michael Merzenich, PhD.
Press Contact
Posit Science PR Team
media@brainhq.com
 | Kevin McGrew (@iqmobile) |
Problems with #bifactor #intelligence #IQ test research studies. #gfactor may not represent a real thing or ability but may be an #emergent factor...like #SES or #DJI. #g and primary abilities uncorrelated....seriously????? Bifactor models are theoretically #agnostic pic.twitter.com/Go77F32UTI | |
Levels of #intelligence research and explanation. Part of my #CHC theory update presentation at #FASP2018 this coming week. #brain #brainnetworks #neuroscience #psychometrics #IQ

 | Kevin McGrew (@iqmobile) |
#runningwithscissors #CHC theory update next week at #FASP conference is when I tackle the #bifactor #allyouneedisg #ghadist negative #IQ test research for the first time. A wild romp in the research. pic.twitter.com/X1gNJu1FPO | |









___
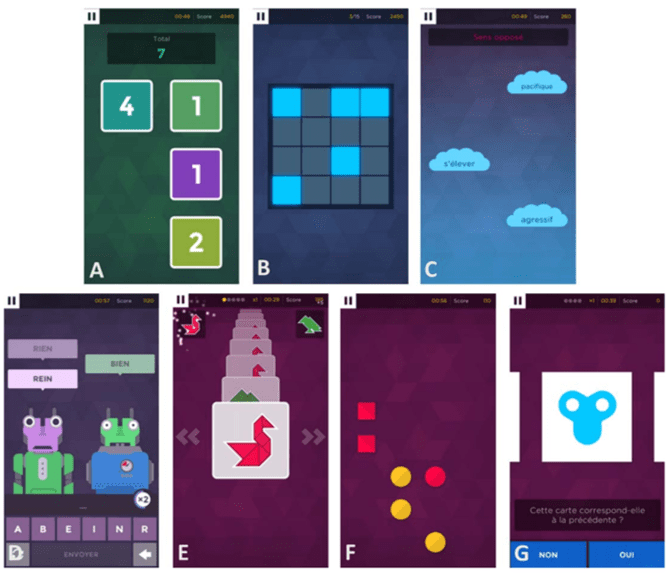
The Use of Mobile Games to Assess Cognitive Function of Elderly with and without Cognitive Impairment (Journal of Alzheimer's Disease):
Abstract: In the past few years numerous mobile games have been developed to train the brain. There is a lack of information about the relation between the scores obtained in these games and the cognitive abilities of the patients. The aim of this study was to determine whether or not mobile games can be used to assess cognitive abilities of elderly. Twenty healthy young adults, 29 old patients with cognitive impairments (Mini-Mental State Exam (MMSE) [20- 24]) and 27-aged controls participated in this study. Scores obtained in 7 mobile games were correlated with MMSE and the Addenbrooke's Cognitive Evaluation revised (ACE-R). Statistically significant differences were found for all games between patients with cognitive impairments and the aged controls. Correlations between the average scores of the games and the MMSE and ACE-R are significant (R = 0.72 [p < 0.001] and R = 0.81 [p < 0.001], respectively). Scores of cognitive mobile games could be used as an alternative to MMSE and ACE-R to evaluate cognitive function of aged people with and without cognitive impairment at least when MMSE is higher than 20/30.

By Alex Fradera
The number of psychiatric diagnoses keep on growing, with perhaps ten times as many categories now as there were 50 years ago. This may in part reflect our growing knowledge, which is welcome. But the sheer density of diagnoses makes it difficult for researchers or clinicians to see the wood for the trees, and it encourages them to settle into silos. It would be advantageous for clinical research and practice if we could introduce some elegance to our understanding. A recent movement in psychology and psychiatry is seeking to do exactly this. It follows evidence that, in the words of US psychologists Robert Kruger and Nicholas Eaton in their 2015 review, "many mental disorders are manifestations of relatively few core underlying dimensions." In the latest foray from this movement, the Journal of Clinical Psychology has published a review outlining another potential core feature: the repetitive occurrence of negative thoughts.
The proliferation of psychiatric diagnoses was baked in from the beginning. Modern psychiatry sought to apply the burgeoning medical model to the mind, treating madness as illness. Physical illnesses are considered as discrete categories, even if they produce overlapping symptoms like a fever, because we can point to their distinct microbial origins.
This has influenced how we approach mental health, meaning someone struggling could be diagnosed with a phobia and also with an eating disorder and maybe separately with depression (and anxiety, and another eating disorder, and another phobia, and OCD…ad infinitum). We bracket these issues out as if they each originate from their own unique strain of mind bacteria. But mental disorders are rooted in dysfunctional mental processes, of which there are only so many. If we put aside the disease model and look for these processes, maybe we can get to a more solid and elegant foundation.
One example would be internalising-externalising. In internalising disorders such as depression, OCD, anxiety and bulimia, the individual tends to draw problems inwards to an inappropriate degree; issues are suppressed or privately managed using ineffective or unhealthy strategies. Meanwhile, externalising disorders like pyromania, kleptomania, and conditions like oppositional defiant disorder or conduct disorder, all involve manifesting problematic thoughts or emotions by projecting them onto the world.
According Kruger and Eaton's landmark review, these aren't just convenient labels: they may actually be more informative than the specific diagnoses. For instance, suicide risk may be better predicted by internalising in all its forms than a specific diagnosis like depression. Similarly, externalising behaviour of any kind is a strong predictor of other forms of externalising, suggesting that it might sometimes be useful to think of the problem as externalising, which can manifest in different ways depending on contextual factors.
Still, this division is too simple to explain everything about mental health. But in interaction with some other features, perhaps we can start to arrive at a complete model that cuts across diagnostic categories while also capturing the richness of psychiatric conditions. What other relevant factors are there? We recently covered work that suggested another potential trans-diagnostic structure: meta-cognition, the ability to judge your cognitive ability. People who were more anxious or depressed showed more accuracy, but less confidence, in how they judged their performance on a mental task, whereas those who tended towards compulsive behaviour (such as those with schizophrenia or OCD) showed overconfidence and did less well. In our piece we described how this pattern can account for patterns of behaviour found in the real world, such as pessimism and jumping to conclusions, respectively.

Now in the most recent example, Deanna Kaplan and her team at the University of Arizona suggest another trans-diagnostic feature: "maladaptive repetitive thought". This is found across many mental health disorders, typically accompanied by a sense that the thoughts are uncontrollable, a negative flavour, and a fixation on seeking rather than solving problems. Consider the ruminative thoughts that characterise depression, the worries that surge up in anxiety, and the obsessive thoughts that drive OCD. Kaplan's team suggest that these different manifestations should be thought of as variations on a key theme, often differing simply in whether the thoughts are focused on the past, present or future.
The researchers note that their model helped them to draw connections to other related phenomena such as the problematic grief phenomenon of yearning, which pulls you into the past towards a desire that cannot be satisfied. They also see parallels in somatic hypervigilance, the constant monitoring of bodily sensations for any cause for alarm. Again, the same features come up: negative valence, uncontrollability, and seeking of problems, in this case in the present moment.
It's not news that unwelcome thoughts are a frequent feature of poor mental health. But as with the internalising and externalising dimensions, it's possible that grouping mental health problems that share repetitive thought processes could offer fresh way of looking at the root causes of people's difficulties. It could be that the core problems driving all psychological disorders are countable on our fingers – if so, and if we can identity these core processes, then it will be easier to understand how they develop, and to apply advances from one area of treatment to another, as well as to see when doing so would be ill-advised.
For example, consider how the three features of internalising/externalising, meta-cognitive judgment and repetitive thought processes could be used to organise our understanding of the recently proposed diagnostic category of maladaptive daydreaming, whereby people are compulsively drawn to their daydreams at the cost of their psychological health. This certainly seems to involve internalising, and could involve overconfident misjudgment of whether the daydreaming is beneficial. And what is a daydream if not an extended, imagistic form of thought (much like a yearning)?
I believe we may be on the verge of a real advance in psychiatry, akin to the turn from individual symptoms to mental syndromes we made one hundred years ago. By looking past surface issues and gripping the fundamental mental processes that drive confusion and distress, we might be better placed to remedy them.
Alex Fradera (@alexfradera) is Staff Writer at BPS Research Digest
